Half of All Cardiac Arrests Go Unwitnessed
Every year, hundreds of thousands of people around the world experience an out-of-hospital cardiac arrest (OHCA) — a sudden event where the heart stops pumping blood effectively. When this happens, survival depends on a brutally simple chain of events: someone notices, calls emergency services, and starts CPR — ideally within minutes. But in roughly half of all cases, no one is there to witness the arrest [1]. The person collapses alone, and the clock runs out before help arrives.
This is why researchers have been exploring whether wearable devices — the smartwatches millions of people already wear daily — could fill that gap. The idea: use the watch's built-in sensors to automatically detect when a pulse disappears, and immediately alert emergency services with a GPS location, even when no bystander is present.
Several research groups are racing toward this goal. Google's Pixel Watch 3 already has an FDA-cleared loss-of-pulse detection feature, validated in a study published in Nature [2]. The Dutch HEART-SAFE consortium and the DETECT project are developing similar systems using different approaches [3, 4]. But until now, these algorithms had only been tested on simulated cardiac arrests in volunteers, or on artificially induced arrests during medical procedures. No one had documented a wearable detecting a real, spontaneous cardiac arrest as it happened — until this case report [1].
A Samsung Watch Detects a Real Cardiac Arrest
The case involves an 82-year-old patient who was admitted to the emergency department with a severe intracerebral hemorrhage — bleeding inside the brain — with a very poor prognosis. After shared decision-making with the family, palliative care was initiated and life-sustaining treatment was withdrawn. With ethics board approval and consent from the patient's next of kin, researchers from Amsterdam UMC placed a Samsung Watch5 Pro on the patient's wrist approximately 40 minutes after withdrawal of treatment, as part of a feasibility evaluation within the HEART-SAFE project.
At the time the watch was placed, the patient's heart was already beating irregularly (a condition called atrial fibrillation) at just 54 beats per minute, with low blood pressure (90/39 mmHg) and an oxygen saturation of only 34% — far below the normal range of 95–100%. This meant the algorithm would have to work through an abnormal and deteriorating signal from the very start. The patient was simultaneously monitored with clinical-grade hospital equipment: an ECG (electrocardiogram, which tracks the heart's electrical activity), an arterial blood pressure catheter (a thin tube inserted into an artery for continuous, precise pressure readings), and a hospital-grade pulse sensor (known as a photoplethysmograph, or PPG — the same green-light technology used in smartwatches, but in a medical-grade form). Together, these served as the reference standard to pinpoint the exact moment the circulation stopped.
Over the following period, the patient's condition gradually worsened. Approximately three minutes before the algorithm flagged the arrest, a rapid decline set in — the heart rate slowed further and blood pressure dropped steadily. Then the algorithm triggered. At that moment, the hospital ECG showed the heart barely firing — a dying rhythm known as agonal bradycardia — with the monitor displaying a heart rate of 0 bpm. The average blood pressure had dropped to just 9 mmHg, essentially no circulation. The patient was declared dead by a clinician approximately four minutes later.
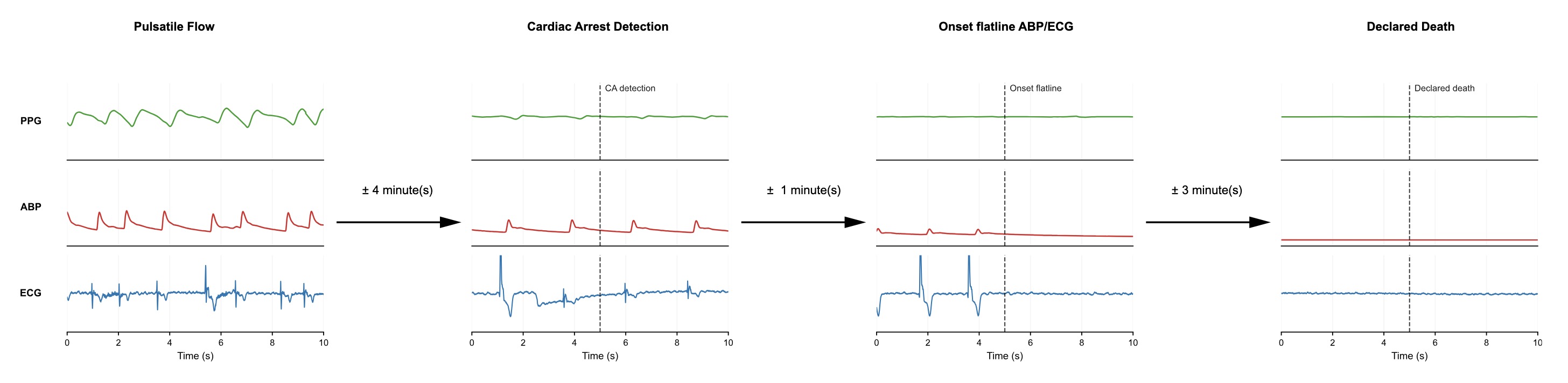
One technical subtlety stands out in the figure above. At the moment of detection (second panel), the hospital's own pulse sensor still registered 28 bpm — picking up residual, weak heart activity. But the smartwatch algorithm correctly interpreted these extremely low-amplitude oscillations as insufficient for effective blood flow and triggered the arrest alert. This is arguably the right call: detecting the point where the circulation has effectively failed — early enough to intervene — rather than waiting for the heart to stop completely. Crucially, no false alarms were generated during the entire observation period.
An important reassurance for the technology's broader applicability: the patient's profoundly low oxygen levels likely did not compromise the smartwatch signal. The green light used by smartwatch pulse sensors absorbs oxygenated and deoxygenated blood similarly, making it relatively insensitive to oxygen changes. This means the approach should remain reliable even when a patient is severely oxygen-deprived.
It's worth noting that the algorithm was applied retrospectively — analyzed after the fact — rather than running live on the watch. The researchers deliberately chose this approach to avoid generating alarms that could disturb the patient's family during palliative care. The patient's family consented to the study, and their contribution made this first-of-its-kind documentation possible.
Why This Matters — and What's Still Missing
To be clear about what this case report is and isn't: it is the first detailed description in peer-reviewed literature of a commercially available smartwatch detecting a spontaneous cardiac arrest that wasn't artificially triggered [1]. It demonstrates that the technology can work on a real event, not just a simulated one. That's a meaningful milestone.
But it's a single case, in a controlled palliative care setting, with a patient whose gradual decline is only one of many ways a cardiac arrest can unfold. In the real world, arrests can be sudden — the heart abruptly entering a chaotic, ineffective rhythm (called ventricular fibrillation) without any warning — or they can be slow-onset, like the progressive deterioration seen here. A viable detection system needs to handle all of these scenarios.
And there's a fundamental tension at the heart of algorithm design: sensitivity versus false alarms. Detecting a cardiac arrest early is critical — every minute of delay reduces survival odds. But setting thresholds too aggressively risks crying wolf, which could overwhelm emergency services and erode user trust. In this case, the algorithm triggered while the heart still had minimal residual activity, which the researchers consider an appropriate detection. But finding the optimal balance across diverse populations and arrest types remains a key challenge.
Real-world use also brings practical complications that a hospital setting doesn't: movement during daily activity creating signal noise, variable watch-wearing habits, diverse skin tones and wrist sizes, and the need to recognize many different types of cardiac events. Importantly, the HEART-SAFE team's algorithm is device-independent — built for any smartwatch running Google's Wear OS, not tied to a single brand [3]. This means it could eventually work across Samsung, Google, and other manufacturers, maximizing accessibility.
Imagine the full scenario working as intended: you're wearing your smartwatch at home, alone. Your heart stops. Within seconds, the watch detects the loss of pulse, confirms you're motionless, and automatically calls emergency services with your GPS coordinates. Nearby trained citizen responders are alerted through networks like the Netherlands' HartslagNu system. Help arrives minutes faster than it otherwise would — potentially turning an unsurvivable event into a survivable one.
We're not there yet. Prospective, real-time testing in everyday environments is the essential next step, along with regulatory approval, integration with existing emergency response systems, and addressing privacy concerns [5]. But this case report — modest in scale, profound in implication — shows that the foundational technology works. The watch on your wrist may not save your life today, but the research is heading in that direction faster than most people realize.
References
- van den Beuken WMF, Tuinman PR, Nideröst B, et al. "First Automated Detection of a Cardiac Arrest Using a Commercially Available Smartwatch: A Case Report", Resuscitation Plus 28 (2026) 101247. https://doi.org/10.1016/j.resplu.2026.101247
- Shah K, Wang A, Chen Y, et al. "Automated Loss of Pulse Detection on a Consumer Smartwatch", Nature 642 (2025) 174-181. https://doi.org/10.1038/s41586-025-08810-9
- van den Beuken WMF, Nideröst B, Goossen SA, et al. "Automated Cardiac Arrest Detection and Emergency Service Alerting Using Device-Independent Smartwatch Technology: Proof-of-Principle", Resuscitation 213 (2025) 110657. https://doi.org/10.1016/j.resuscitation.2025.110657
- Edgar R, Scholte NTB, Ebrahimkheil K, et al. "Automated Cardiac Arrest Detection Using a Photoplethysmography Wristband: Algorithm Development and Validation in Patients With Induced Circulatory Arrest in the DETECT-1 Study", The Lancet Digital Health 6 (2024) e201-e210. https://doi.org/10.1016/s2589-7500(23)00249-2
- van den Beuken WMF, van Schuppen H, Demirtas D, et al. "Investigating Users' Attitudes Toward Automated Smartwatch Cardiac Arrest Detection: Cross-Sectional Survey Study", JMIR Human Factors 11 (2024) e57574. https://doi.org/10.2196/57574
